Never Fall Behind Webinar Follow-Up FAQ with Dr. Emily & Dr. Jin Lee
Q: Are there recommendations from the AAP for developmental screening and surveillance? Can you clarify these guidelines?
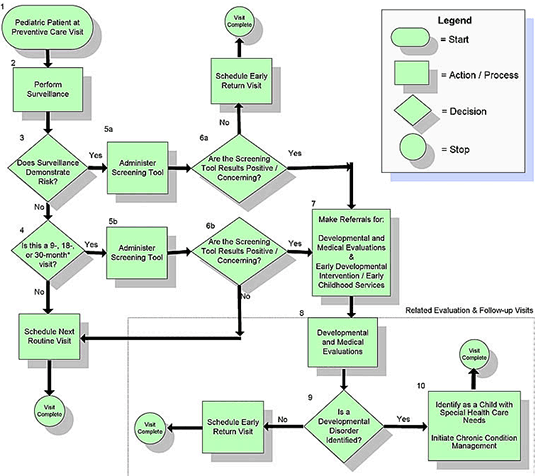
A: Dr. Jin Lee: The AAP recommends developmental surveillance at every single well-child visit. What they call developmental surveillance/surveillance is basically another word for developmental monitoring. In contrast, developmental screening requires using a structured, formal screening tool that’s validated such as PEDS, ASQ, and others specified on the AAP website at 9, 18, and 30 months. Screening for autism should take place at 18 and 24 months.
Check out our blog on the roles of screening and surveillance in developmental monitoring.
Q: Is there a minimum age for neuropsychological testing? Would babies who suffer neonatal abstinence syndrome be a candidate for this or would standard developmental screening and surveillance suffice?
A: Dr. Emily: There really isn’t a minimum age requirement for a neuropsych evaluation. Prior to going into private practice, I spent time working in a neonatal intensive care unit (NICU) and saw little ones as soon as they were born in order to begin this process of monitoring development closely. Of course, there is a huge range in terms of what you can screen for depending on a child’s age. With infants, there is a lot less that you are expecting them to do, and can, therefore, screen for, compared to older children. But, there really isn’t a minimum age at which a neuropsychological evaluation becomes appropriate or at which point it is appropriate to involve a neuropsychologist. What is often a limiting factor is that there are a lot of neuropsychologists who have not undergone training in how to work with infants or very young children. This is why you may sometimes come across providers who say they will not work with a child until about 4 or 5 years of age. I think this is a shortcoming with a lot of providers in my field because we know that working with children from a very very young age is incredibly important to make sure that we are setting them up to be on the right developmental track.
In terms of the second part of the question, children who are undergoing withdrawal from substances that they were exposed to in utero are at high risk of experiencing developmental issues. As such, it will be important to monitor their development closely. In my experience, these infants are also often irritable, which also makes parenting much more of a challenge. I think that it’s also really good to involve a neuropsychologist, again, early on, to help monitor development. As I mentioned, there are tests that allow us to measure skills in infants that begin at birth and allow us to monitor development moving forward. This close monitoring, especially during those early childhood months and years, really allows us to make sure that we’re not running into any developmental hiccups. What I often see with families when they’ve had a baby in the NICU is that once they are discharged from the NICU they have this idea often that they are out of the woods developmentally, that their child is now healthy enough to go home. They often have a very limited understanding or awareness of some of the developmental risks that may be associated with any medical issues or, indeed, just with premature birth in and of itself.
Q: A challenge when taking action early is that, when referrals are made, many of these kids do not qualify for early intervention. This causes a lot of anxiety for parents during the waiting period for rescreening. What sorts of actions would you recommend during the waiting period?
A: Dr. Lee: I have a daughter who is 22 months ago and a few months ago she was diagnosed with speech delays, at low risk. This diagnosis was made only after I pushed for an evaluation through my pediatrician, who didn’t believe she was delayed. I insisted and then I actually self-referred myself to a regional center in CA, a free intervention center offered by the state. They are required by law within 45 days to see my child because I have given them an issue of concern. So I always recommend folks to refer themselves to these centers.
14% of children are low risk for developmental delays, and in my case, the regional intervention center gave me 5 pages of activities that I can do to practice different ways of speaking with my 22-month old daughter in a way that is fun and activity-based. Without self-referring myself to that center, I would not have gotten that information because the information I initially was given by my doctor was only a page, not nearly enough for an anxious mom like myself. At BabyNoggin, which I am the founder of, we have incorporated a lot of these activities within the app, so that when parents go through the app and screen their kids and find out their kids are either low, medium, or high risk, we actually provide recommendations for the parents on what to do next. For low and medium kids we typically give their parents activities to do and, for those at high risk, we give their parents phone numbers and addresses for their early intervention services nearby them so that they can self-refer.
A: Dr: Emily: This is something that is a major source of frustration for me. Often, when we are looking at the denial of a delay or somebody saying that a delay is not significant enough, it is usually government-based agencies that are doing this, whether it is an early intervention program or whether it is school-based services when a child is 3 or older. A lot of these denials stem from children not meeting thresholds that have been somewhat arbitrarily set for what’s considered a delay and what isn’t. A lot of my frustration around that tends to be that the cut-off points that are considered are really not grounded in scientific data. School systems and early intervention programs tend to wait until a delay is hugely evident before they will actually jump in and do something about it. So they are essentially waiting for a child to fail before they feel that the evidence is substantial enough for them to intervene. As you have probably seen now from what Dr. Lee and I have talked about, this is not something that is backed up by the research at all. The research really says that we need to intervene as soon as possible. In addition to pursuing the supports available through early intervention programs or the school system, I encourage families to pursue private evaluations (through their health insurance or private pay) because you’re going to get a more thorough and complex screening by somebody who knows that even if a delay is not critical, that there’s often a lot that we need to do to help ensure it does not become critical.
Q: What parents should do when regional centers do not assess within 45 days?
Dr. Lee: I’m based in San Francisco, where there is a family advocacy group locally, called Support for Family, and they usually train families saying when it’s close to maybe 35 days, 40 days, and you haven’t received a call or email from the local regional center or wherever your early intervention service might be to gently call or email and say, “Hey, I know the 45 day deadline is coming up, I just want to check in and see what the status of my child is.” Just give them a gentle reminder, because, if you empower yourself with the legal implications, they will feel a little bit more threatened and want to help. They are flooded with concerns all the time, which is why it’s many times difficult to meet that 45-day deadline. However, when they do not meet it, they are given a lower score in when they are given an annual performance review by the state, which typically means lower funding dollars to them. So, they absolutely want to do everything they can to meet the 45 days, but just be mindful that it might not happen all the time. I know in San Francisco, especially at the beginning and end if the school year, they get super busy. In the summer and holiday season they are not as busy, so you might be able to get the kids in earlier.
Q: What kinds of things are done in ABA therapy?
Dr. Emily: ABA or applied behavior analysis therapy is an approach that is taken to help support development in children with autism. There is a fair amount of research that it is an effective intervention for decreasing problem behaviors and increasing behaviors that you want to see more often (for example, communicating). ABA is a very structured way of interacting with children to help teach them the link between their actions and the responses of others. It’s a very repetitive approach to building skills that emphasizes reinforcing the behaviors that you do want to see and practicing that behavior until it becomes more and more automatic. While there is a lot of data out there suggesting it is beneficial for autism, it actually has a number of appropriate applications for children with other developmental issues as well. In fact, it’s one of the first-line treatments recommended by the American Academy of Pediatrics for children under the age of 5 years who have been diagnosed with ADHD. Here, it can help with some of that behavioral and emotional regulation that young children with ADHD will sometimes struggle with. It can also be a helpful intervention for children who have intellectual disabilities or who have substantial language delays where again that kind of structure and consistency is often really important in helping them make progress.
Q: What suggestions are there for how to present these services without triggering resistance within the stigma of developmental delays?
Dr. Emily: I think this is where apps like BabyNoggin can play a big role because if parents are tracking development closely, they will be the ones who bring up developmental concerns to you. When a situation arises where you, as a provider, have concerns that are not shared by the parents, I think you need to discuss your concerns. Sometimes, parents may not have concerns because this is their first child and they may not have much awareness of what typical development looks like. Here, as a provider, part of your role is to start to gently introduce a family to what you are seeing (or not seeing). Once you start this conversation, you may find that a family is very receptive to taking steps to help establish if delays are present. If you encounter some resistance, then it may take your bringing this up several times to the family across several different visits and also providing them with information about child development before they are ready to take the next step.
Q: For pediatricians moving to a new state where would be a good place to start investigating community resources for parents with kids with delays?
A: Dr. Lee: For children 0-3 years old, contact your local early intervention system to find out about community intervention resources. You can find your state’s early intervention contact information here. To learn more about early intervention for children under 3, click here. For children 3 years old or older, contact your local public school system. To learn about the available services and process for children over 3, click here.
Q: Does early intervention exist for anxiety disorders and if so, what does it look like?
A: Dr. Emily: There really isn’t an established protocol for how to address early signs of mood disorders (e.g., anxiety, depression) in young children. As with many conditions, a child is at higher risk of developing a mood disorder if family members also have the condition. This means that you need to watch for signs of an emerging mood disorder and take prompt action if you see concerns.
- First, it’s important to try to get an accurate diagnosis from an experienced provider if you start to see that your child’s mood is interfering with their ability to do things that their peers are doing. Mood disorders are sometimes misdiagnosed as other conditions. For example, some children with social anxiety are misdiagnosed with autism.
- Then, you want to clearly identify what is triggering mood concerns. Social difficulties, unrecognized learning problems, and unrealistic expectations can all trigger mood issues and warrant very different interventions.
- Finally, you want to implement an intervention plan. The type of intervention recommended will depend on your child’s age and also what is triggering their mood concerns. In young children, intervention might take the form of behavioral therapy or play therapy, in older children cognitive-behavioral therapy often is recommended.
If your child is not yet showing significant signs of anxiety, one of the things that you might want to do is look at ways to help your child develop a healthy relationship with anxiety so that it is something that does not limit their progress. For example, work on praising your child for the effort that they put into something rather than the outcome. Similarly, celebrate your child trying new things even if they do not necessarily succeed. Having a whiteboard at home where everyone can write down the new things that they have tried can be a fun way to celebrate times when your child pushes through anxiety to try something new.
Pay attention to how you express your emotions. Model what it is like to make and recover from mistakes (for example, overcooking dinner or forgetting to pay a bill on time) in a healthy way. This can help normalize the experience of making mistakes for your child. You can also look for safe opportunities that can help your child learn that it is okay to fail. Playing board games or family sports games can be great ways to do this. You can model how to cope with losing or missing a shot and give your child practice managing these things as well. When your child is distressed, it’s perfectly appropriate to validate their feelings of distress, but you also want to encourage them to push through the disappointment and try again.
Dr. Emily is an Oxford-trained, board-certified neuropsychologist. Dr. Emily is an expert in child development and brain function and has a practice in Atlanta working with infants and children who are at-risk of (or have) developmental delays or complex medical issues. She has published research on supporting quality of life in children and on the cognitive strengths and weaknesses of children with medical conditions including epilepsy, brain tumors, and genetic disorders. For more information about Dr. Emily and the work she is doing, visit BabyNoggin.com
Dr. Jin Lee is the CEO of BabyNoggin. She is an Oxford-trained child psychologist and has over a decade of experience in healthcare, innovation, and research. She has worked in the innovation and venture arms of Humana and Providence St. Joseph Health. Dr. Lee has been featured on numerous healthcare blogs and has showcased her work at multiple child health-related conferences such as the Aspen Institute Children’s Forum and National Early Head Start. To learn more about Dr. Lee and the work she is doing, visit DrEmilyNeuropsych.com.